面對醫療系統的挑戰
人力不足與醫療失誤的危機
面對醫療系統的挑戰
人力不足與
醫療失誤的危機
醫療系統危機的深度解剖
人力短缺
2026年,美國將面臨320萬名醫療提供者的短缺,台灣每年兩百萬次手術麻醉卻只有800名職業麻醉醫生。
延誤診斷與治療
缺乏足夠專業人員即時介入,導致醫療負擔和疏失增加,患者的死亡率上升。
醫療支出倍增
因為可近性不足,患者只能選擇更昂貴且保守的處理方式,加劇醫療支出負擔。
我們致力於運用人工智慧技術,將主觀的聽診數據轉換為客觀且連續的資訊,增進溝通效率、減低失誤與人力負擔。
榮譽事蹟

2019.01
RESI Innovation Challenge
新創挑戰賽第二名

2020.01
AWS 創新者聯盟 2 Demo Day
最佳技術獎

2020.09
數位時代
年度最具成長潛力新創

2019.01
RESI
Innovation
Challenge
新創挑戰賽
第二名

2020.01
AWS
創新者聯盟
2 Demo Day
最佳技術獎

2020.09
數位時代
年度最具
成長潛力新創

2019.01
RESI Innovation Challenge
新創挑戰賽第二名

2020.01
AWS 創新者聯盟 2 Demo Day
最佳技術獎

2020.09
數位時代
年度最具成長潛力新創

2020.12
第17屆國家新創獎
2021.12
衛福部藥物科技研究發展獎
銅質獎

2021.12
第3屆美國高通
台灣創新競賽第二名

2020.12
第17屆
國家新創獎
2021.12
衛福部
藥物科技
研究發展獎
銅質獎

2021.12
第3屆
美國高通
台灣創新競賽
第二名

2020.12
第17屆國家新創獎
2021.12
衛福部藥物科技研究發展獎
銅質獎

2021.12
第3屆美國高通台灣創新競賽
第二名

2022.03
Select USA AIT MedTech
冠軍

2023.11
第30屆中小企業創新研究獎
2024.6
Entrepreneurial Champions
Award

2022.03
Select
USA AIT
MedTech
冠軍

2023.11
第30屆
中小企業
創新研究獎
2024.6
Entrepreneurial
Champions
Award

2022.03
Select USA AIT MedTech
冠軍

2023.11
第30屆中小企業創新研究獎

2024.6
Entrepreneurial Champions
Award
2024.06
經濟日報創業之星選秀大賽
優勝
2024.8
新創100大
2025
To Be Continue...

2024.06
經濟日報創業之星選秀大賽
優勝

2024.8
獲評選為新創100大

2025
To Be Continue...
早期診斷與即時警示
提早發現問題,並提供即時警示,
幫助醫療專業人員做出更快的反應。
早期診斷與即時警示
提早發現問題,並提供即時警示,幫助醫療專業人員做出更快的反應。
早期診斷與即時警示
提早發現問題,並提供即時警示,幫助醫療專業人員做出更快的反應。
長期追蹤與靈敏偵測
長期病患追蹤及高靈敏偵測方面的應用,
特別是針對結構性心病、睡眠呼吸中止症等慢性疾病的偵測。
長期追蹤與靈敏偵測
長期病患追蹤及高靈敏偵測方面的應用,特別是針對結構性心病、睡眠呼吸中止症等慢性疾病的偵測。
長期追蹤與靈敏偵測
長期病患追蹤及高靈敏偵測方面的應用,特別是針對結構性心病、睡眠呼吸中止症等慢性疾病的偵測。
AI醫療技術的市場機會
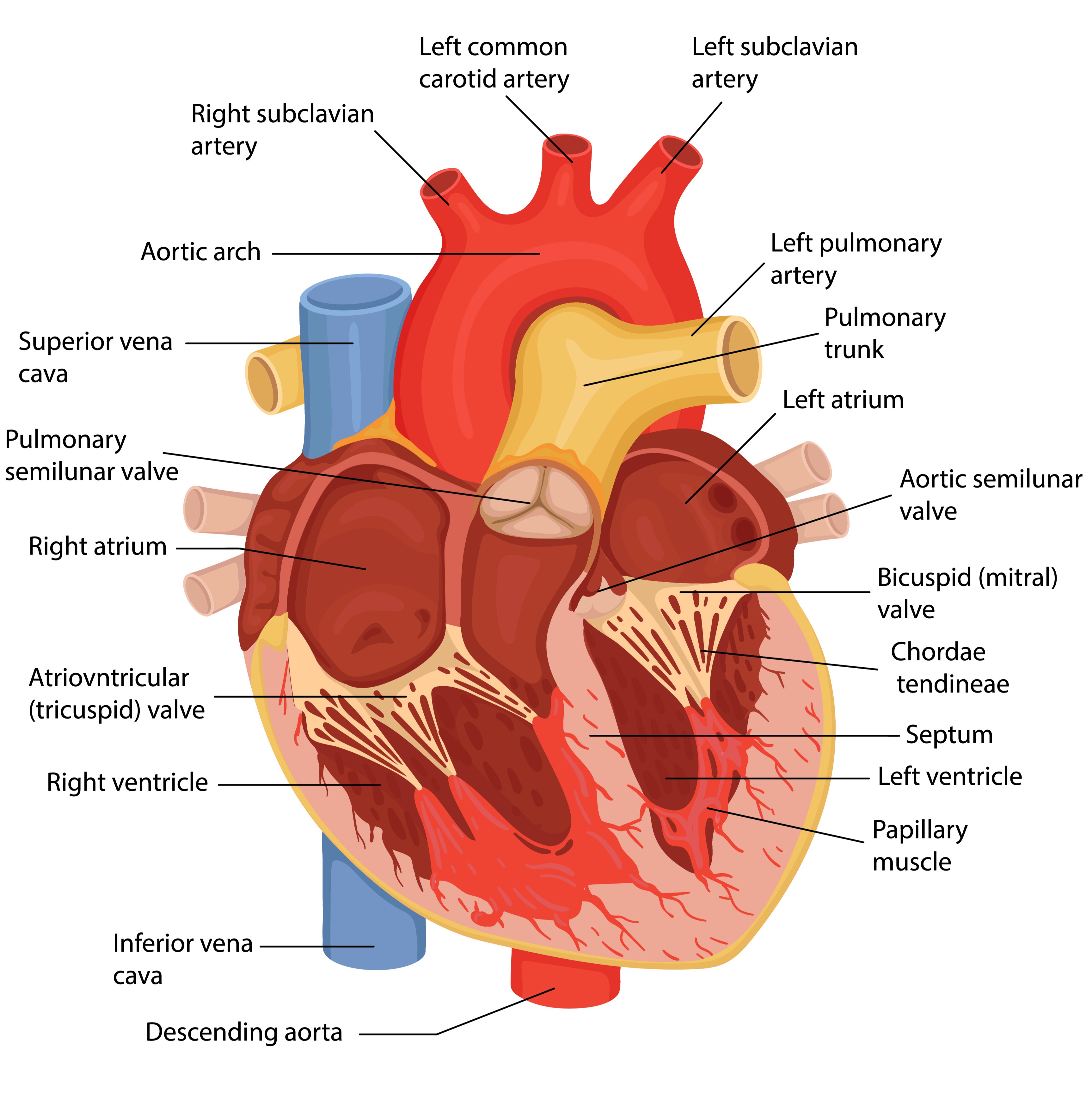
結構性心病
六千四百萬個
可能病患
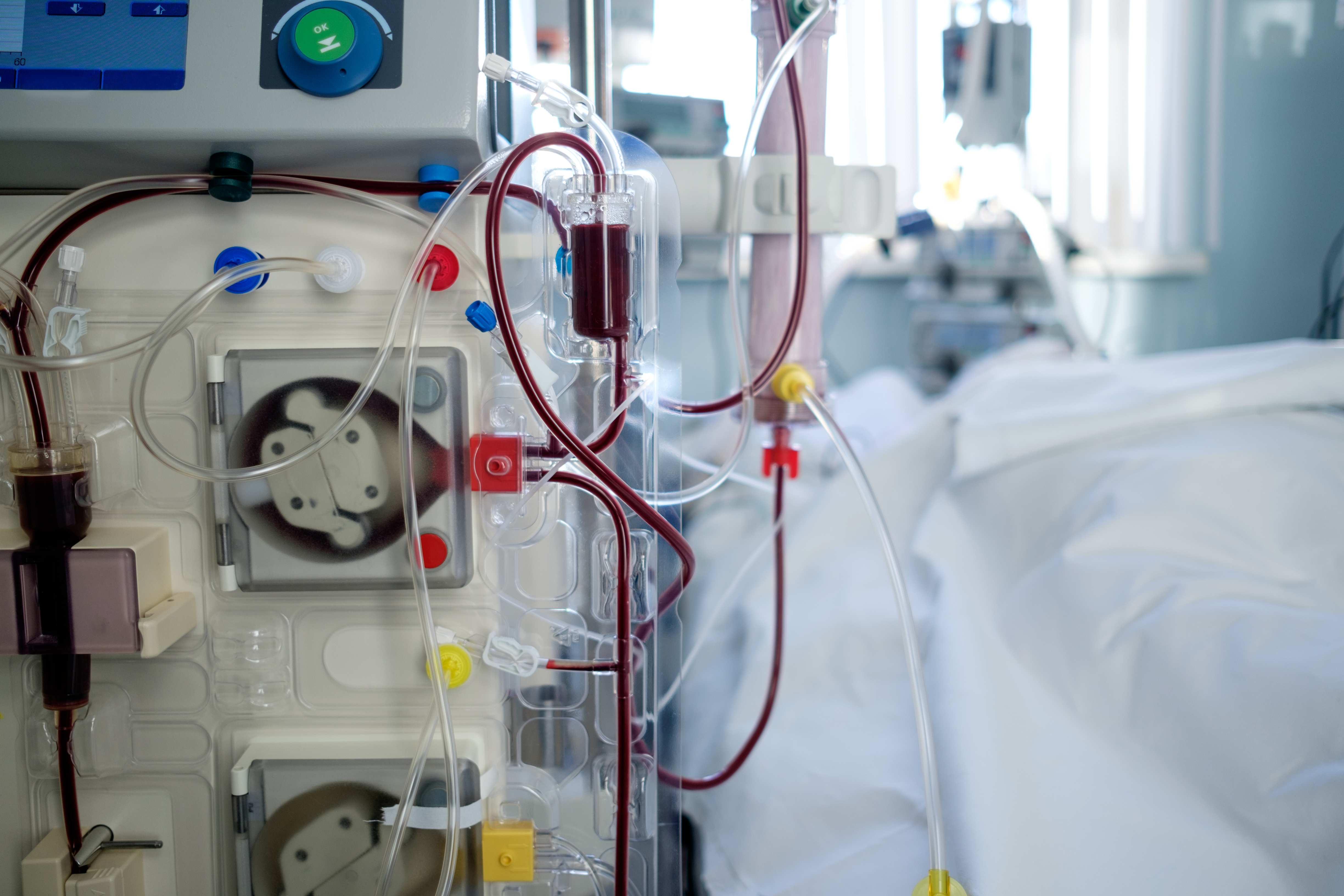
血液透析
血管阻塞
八億四千萬人次
有血液透析需求
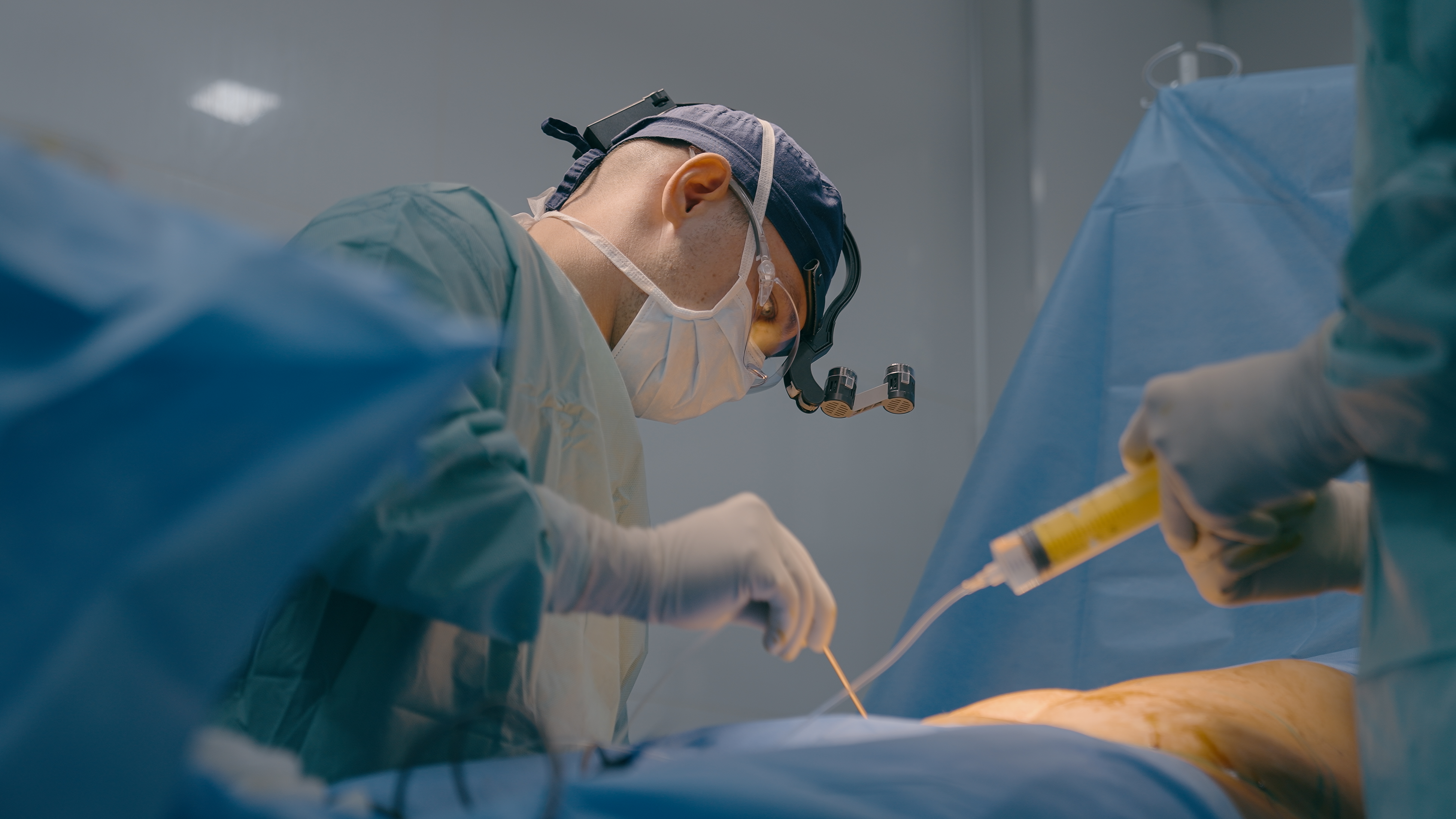
麻醉鎮靜安全
每年約一億人次手術鎮靜麻醉
26億美元市場機會

阻塞型
睡眠呼吸中止症
九億三千萬人次受苦
90億美元高額成長

結構性心病
六千四百萬個
可能病患

麻醉鎮靜安全
每年約一億人次
手術鎮靜麻醉
26億美元市場機會

血液透析
血管阻塞
八億四千萬人次
有血液透析需求

結構性心病
六千四百萬個
可能病患

血液透析、
血管阻塞
八億四千萬人次
有血液透析需求

麻醉鎮靜安全
每年約一億人次
手術鎮靜麻醉
26億美元市場機會

肺部疾患
五億九千萬病人
有長期追蹤需求

血液透析
血管阻塞
八億四千萬人次
有血液透析需求

麻醉鎮靜安全
每年約一億人次手術鎮靜麻醉
26億美元市場機會

阻塞型
睡眠呼吸中止症
九億三千萬人次受苦
90億美元高額成長

肺部疾患
五億九千萬病人
有長期追蹤需求

阻塞型睡眠呼吸
中止症
九億三千萬人次受苦
90億美元高額成長

血液透析
血管阻塞
八億四千萬人次
有血液透析需求

阻塞型睡眠呼吸中止症
九億三千萬人次受苦
90億美元高額成長

肺部疾患
五億九千萬病人
有長期追蹤需求

麻醉鎮靜安全
每年約一億人次
手術鎮靜麻醉
26億美元市場機會